Featured Topics
Featured Products
Events
S&P Global Offerings
Featured Topics
Featured Products
Events
S&P Global Offerings
Featured Topics
Featured Products
Events
S&P Global Offerings
Featured Topics
Featured Products
Events
Financial and Market intelligence
Fundamental & Alternative Datasets
Government & Defense
Professional Services
Banking & Capital Markets
Economy & Finance
Energy & Commodities
Technology & Innovation
Podcasts & Newsletters
Financial and Market intelligence
Fundamental & Alternative Datasets
Government & Defense
Professional Services
Banking & Capital Markets
Economy & Finance
Energy & Commodities
Technology & Innovation
Podcasts & Newsletters
24 Apr, 2026
By Tom Jacobs
UnitedHealth Group Inc.'s stock had a strong week highlighted by a positive earnings outlook for the remainder of the year and a nationwide expansion of the insurer's rural health care initiatives.
The Eden Prairie, Minnesota-based carrier's stock improved 9.2% for the week as of market close on April 23. Fueling that rise was the insurer's first-quarter earnings released on April 21, which included an increase in its full-year adjusted earnings per share guidance to $18.25, from $17.75 presented earlier in the year.
At the same time, United announced on April 20 that it was eliminating most medical prior authorizations for key rural care hospitals and providers nationwide, as well as accelerating payments to those hospitals. S&P Global Ratings analyst Francesca Mannarino said the move is a continuation of the company's support for independent hospitals and physicians.
"If [the hospitals and providers] remain independent, the expectation is that they may be essentially more challenged on cash flow and are looking for that timely payment," Mannarino said in an interview. "Improved prior authorization has been one of their focal points to make sure people are getting the care that they need."
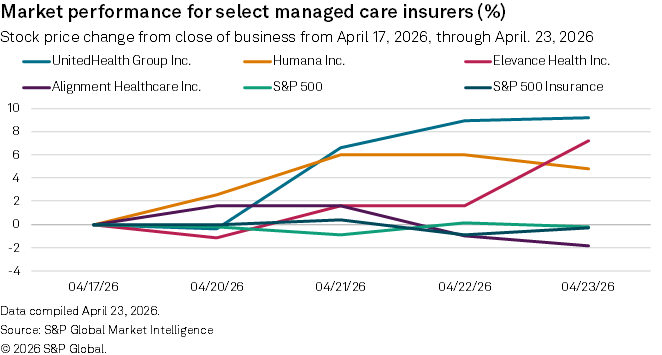
Stock results for other carriers in the managed care sector were mixed for the week. Elevance Health Inc. and Humana Inc. were up 7.2% and 4.8%, respectively, while Alignment Healthcare Inc. fell 1.8%. The S&P 500 was down 0.2% over the same period, while the S&P 500 Insurance Index was off 0.3%.
United's rural initiative
UnitedHealth's plan for rural providers includes speeding payments by up to 50% for approximately 1,500 rural hospitals and all Critical Access Hospitals, and exempting rural providers from most medical prior authorization requirements across all lines of business. Also included is the launch of new hub-and-spoke partnerships, which are characterized by a main healthcare campus that receives resources and supplies to support intensive medical services, and several surrounding facilities that provide more limited services.
Timothy Noel, CEO of UnitedHealthcare Business, said during the company's first-quarter earnings call the initiative is part of UnitedHealth's intensified efforts to support rural health care providers.
"All these efforts and others like them are part of our commitment to pursue and invest in new and innovative ways to fulfill our mission to help people live healthier lives and help make the health system work better for everyone," Noel said.
UnitedHealth did not respond to a request for further comment.
Other managed care companies are supportive of independent providers, said S&P Global Ratings analyst James Sung, because they prefer working with a diverse group of providers rather than a concentrated provider market.
"The rural aspect is just a little bit more pronounced because there's less diversity and fewer options for access for some of their members," Sung said in an interview. "That is important because when you have a health insurance product, you need it to be supported by access to actual providers."
Mannarino said the changes in prior authorization procedures are important because they help eliminate fraud, waste and abuse when an insured does not necessarily need a service.
"There is a balance to it, to the extent that they can actively focus on reducing the frustration in the sector across patients and providers," Mannarino said. "That is definitely one of the keen focal points that [UnitedHealth] is pursuing this year."
Growth in April
United's stock has risen 26% since April 6, when the Center for Medicare and Medicaid Services approved a 2.48% net average rate increase for Medicare Advantage payments in 2027. Participating insurers were thrown a curveball by CMS on Jan. 26 when it initially published a proposed 0.09% rate increase, while insurers and analysts had been anticipating a 4% to 6% rate hike.
Sung said UnitedHealth is improving from an earnings perspective, but the recovery is still early and may take some time.
"One thing that could have thrown off the recovery would have been if CMS had kept the Medicare Advantage rate where it originally proposed," Sung said. "[The 2.48% increase] eases some of the pressure for '27, and it just a little bit better of a path for the earnings recovery for this company."