Featured Topics
Featured Products
Events
S&P Global Offerings
Featured Topics
Featured Products
Events
S&P Global Offerings
Featured Topics
Featured Products
Events
S&P Global Offerings
Featured Topics
Featured Products
Events
Financial and Market intelligence
Fundamental & Alternative Datasets
Government & Defense
Professional Services
Banking & Capital Markets
Economy & Finance
Energy & Commodities
Technology & Innovation
Podcasts & Newsletters
Financial and Market intelligence
Fundamental & Alternative Datasets
Government & Defense
Professional Services
Banking & Capital Markets
Economy & Finance
Energy & Commodities
Technology & Innovation
Podcasts & Newsletters
01 May, 2026

By Tyler Hammel
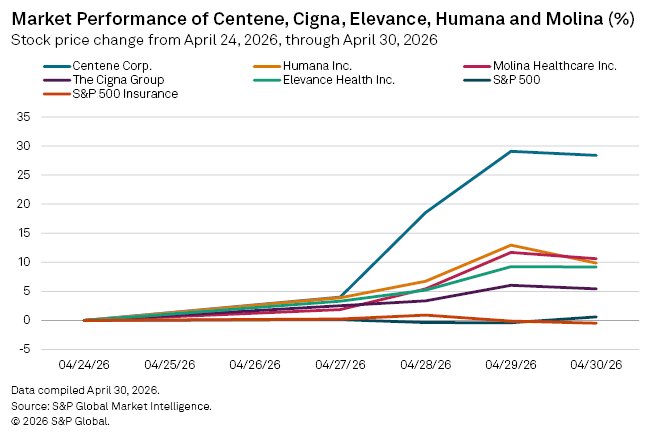
US health insurers have made notable gains on Wall St. following a series of earnings call that presented better than anticipated results, outpacing both the wider insurance sector and the broader market.
The sharpest rise was by Centene Corp., which saw its stock rise 29.1% through close of trading Thursday since April 24 when earnings season for US insurers kicked off. Fellow managed care insurers Humana Inc., Molina Healthcare, Inc., Elevance Health Inc. and The Cigna Group also saw notable rises since their first quarter earnings calls.
These increases outpaced both the S&P 500 and S&P Insurance Index, which rose 0.61% and fell 0.47% during the period, respectively.
Membership shifts
A major focus of Centene's first quarter earnings call was its better than expected ACA marketplace membership retention, which contrasted with comments made the month prior.
Following the loss of Affordable Care Act (ACA) tax credits in the fourth quarter of 2025 amid political wrangling in Congress, Centene experienced significant membership contraction due to its higher relative concentration of members who bought ACA plans through the public marketplace, CEO Sarah London said. However, the shift also drove some members to drop from higher silver tier plans to lower-cost bronze tier plans, altering the risk pool and leading to higher costs in the silver tier, London said.
However, London said the nature of the ACA marketplace plans abates some of this concern.
"It is important to note that in other insurance markets the concept of adverse selection can be scary, but that's not actually the case in marketplace because ... the risk adjustment mechanism is specifically designed to counteract adverse selection," London said. "And often, it can actually be a profitable strategy to care for sicker members in this market."
J.P. Morgan analyst Scott Stansel echoed London's comments, pointing to an April report from the Wakely Consulting Group which examined the shifts in ACA marketplace plans in 2026.
"When the Wakely data were released, we noted that the estimate for the market to decline by -17% to -26% in 2026 was somewhere between in line to slightly better than expected, and we felt Centene's commentary supported this thesis," Stansel wrote.
However, Stansel also noted the higher acuity of the remaining Silver tier members, describing it as "one of the largest swing factors embedded in [Centene's] guidance."
Humana, which saw a stock bump of 13%, the second largest among managed care insurers, was one of the few insurers in the sector not to raise its 2026 earnings guidance, with CEO Jim Rechtin remarking during an earnings call that the company was where it "expected to be."
The insurer has benefitted from a Medicare Advantage rate increase for 2027 approved by the Centers for Medicare & Medicaid Services, Rechtin said, but also noted that medical cost trends continue to outpace program funding. Humana still expects to double its individual Medicare Advantage margin in 2026, benefitting from expected membership growth.
While it is early in the year, Humana's better than expected medical cost trends across new and existing membership is a positive sign, J.P. Morgan analyst Lisa Gill wrote in a research note.
"To that end, we are not necessarily surprised that Humana did not increase its guidance in [the first quarter] given how early it is in the year and the large cohort of new [Medicare Advantage] enrollees that it has added," Gill wrote.
Lemonade loses some fizz
While managed care insurers broadly saw gains, other insurers saw more mixed results.
Among the biggest stock changes among listed US insurers from April 24 through April 30 was experienced by Lemonade Inc., which saw its stock tumble 14.8% during the period.
The property and casualty insurer reported mixed earnings results, including a net loss of $35.8 million for the first quarter, compared with a loss of $62.4 million a year ago. However, Lemonade showed improvement in several metrics — revenues jumped 70.6% to $258 million, net written premiums more than doubled to $274 million from $115.4 million and in-force premiums rose 32% to $1.33 billion.
The insurer received a "market perform" rating from William Blair analyst Adam Klauber, who wrote that Lemonade's improvements could be tempered in the future by efforts to expand into more complicated markets.
"While we are encouraged by Lemonade's strong premium growth, continued marketing efficiency, and improving underwriting and operational leverage, we see increasing execution risks as it expands into the more competitive and complex auto market and maintain our market Perform rating pending further progress on the auto ramp-up and toward profitability," Klauber wrote.
Similarly, insurance broker Brown & Brown Inc. reported a rise in revenue, but flat organic growth, resulting in its stock declining 6.5% during the period.
Klauber also rated Brown & Brown "market perform," noting that the growth outlook worsened from already low expectations with incremental headwinds from rising costs associated with catastrophe property rates, among other factors.