Featured Topics
Featured Products
Events
S&P Global Offerings
Featured Topics
Featured Products
Events
S&P Global Offerings
Featured Topics
Featured Products
Events
S&P Global Offerings
Featured Topics
Featured Products
Events
Financial and Market intelligence
Fundamental & Alternative Datasets
Government & Defense
Professional Services
Banking & Capital Markets
Economy & Finance
Energy & Commodities
Technology & Innovation
Podcasts & Newsletters
Financial and Market intelligence
Fundamental & Alternative Datasets
Government & Defense
Professional Services
Banking & Capital Markets
Economy & Finance
Energy & Commodities
Technology & Innovation
Podcasts & Newsletters
10 Apr, 2026

By Tyler Hammel
US managed care insurers saw a notable bump to their stock prices this week following news of higher than anticipated Medicare Advantage rates for 2027.
On April 6, the Centers for Medicare & Medicaid Services (CMS) approved a net average rate increase of 2.48%, representing more than $13 billion in additional Medicare Advantage payments to plans for calendar year 2027.
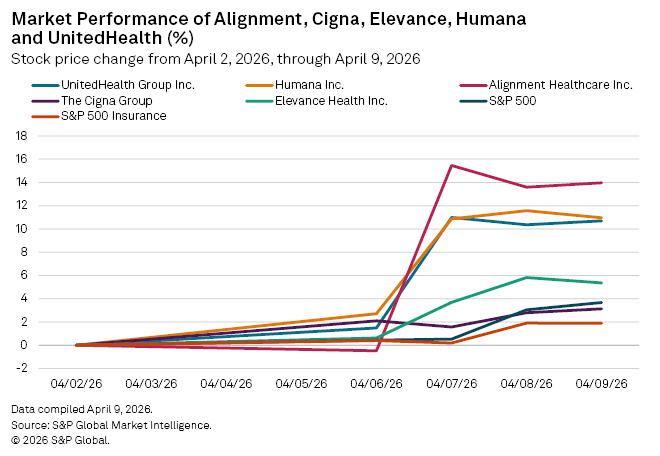
Since April 2, stock prices for major publicly traded managed care insurers have jumped, with Alignment Healthcare Inc. seeing the biggest bump of 14% by close of trading on April 9.
Fellow managed care insurers also saw higher stock prices, with UnitedHealth Group Inc. rising 10.7%, Humana Inc. climbing 11%, Elevance with a 5.4% bump, Centene rising 6.9% and The Cigna Group increasing 3.1%. Of the publicly traded managed care insurers, only insurtech HealthEquity Inc. saw a modest decline in price during the period, falling just 0.6%. Most managed care insurers outpaced both the S&P 500 and the S&P Insurance Index, which rose 3.7% and 1.9%, respectively, during the period.
The higher-than-anticipated Medicare Advantage rates are an indication that CMS is engaging stakeholders, deferring to data and acting rationally, wrote Piper Sandler analyst Jessica Tassan in a research note discussing several managed care insurers, including UnitedHealth and Alignment.
"This does not mean boon times for Medicare Advantage, but it does suggest a period of relative stability conducive to strategic planning and execution," Tassan wrote.
For several months, managed care insurers have faced the grim prospect of near-flat Medicare Advantage rates following an Advance Notice from CMS in January. Medicare Advantage, which offers seniors expanded versions of government-subsidized health plans through partnerships with private insurers, has been a growing cost area for managed care insurers since the COVID-19 pandemic. Costs associated with the plans have increased as seniors delayed seeking care during the pandemic, and managed care companies claim that federally set rate increases have not kept pace.
The increase announced this week reflects factors such as growth rates of underlying costs, 2026 Star Ratings for 2027 quality bonus payments, and risk adjustment updates, according to a news release.
Rising tides
In the current managed care environment, UnitedHealth and Alignment are among the best positioned due in part to their growth potential, according to Tassan.
"We would be buyers of Alignment into that operating environment for upside to earnings from care delivery innovation and accelerating growth," Tassan wrote.
This perspective was partially echoed by J.P. Morgan analyst John Stansel, who wrote in a research note that CMS' final Medicare Advantage rates were a positive surprise, partially mitigating the significantly disappointing Advance Notice in January.
While most investors would prefer higher rates, Alignment is in a better position than other managed care companies to grow enrollment, according to Stansel.
"[With] most [managed care companies] needing to exercise margin discipline (and potentially reduce benefits to achieve that goal), we think this puts Alignment in a position to continue to grow enrollment [more than 20%], while the company has demonstrated that it can improve margins in a worse funding backdrop than 2027," Stansel wrote.
This creates "something of a privileged position for Alignment," Stansel wrote, allowing for rates pressuring margin improvement targets, but not to the extent that Alignment cannot improve its own margins, as its care delivery and stratification approach improves.
Much of this growth is expected to come from several key counties in California where Alignment has a growing presence, Stansel wrote, but several other states present both opportunities and challenges for membership growth.
"New state entry is likely more of a 2028/2029 tailwind as the company scales enrollment, but remains a point to watch in the longer-term enrollment growth target," he wrote.