Featured Topics
Featured Products
Events
S&P Global Offerings
Featured Topics
Featured Products
Events
S&P Global Offerings
Featured Topics
Featured Products
Events
S&P Global Offerings
Featured Topics
Featured Products
Events
Financial and Market intelligence
Fundamental & Alternative Datasets
Government & Defense
Professional Services
Banking & Capital Markets
Economy & Finance
Energy & Commodities
Technology & Innovation
Podcasts & Newsletters
Financial and Market intelligence
Fundamental & Alternative Datasets
Government & Defense
Professional Services
Banking & Capital Markets
Economy & Finance
Energy & Commodities
Technology & Innovation
Podcasts & Newsletters
25 Feb, 2026
By Tom Jacobs and Malik Ozair Zafar
Virginia's health insurance marketplace resilience will be tested by recent challenges, especially the loss of federal subsidies, according to the state's insurance regulator.
The state's Affordable Care Act individual exchange has high participation from carriers and health plans. All 98 counties and 38 independent cities have at least two healthcare plans, with a quarter of them having five plans available.
While that is a good sign of the market's health, Virginia Bureau of Insurance Commissioner Scott White said there are some "concerning" trends, including the declining number of ACA-plan carriers working within the state and the expiration of ACA subsidies.
"You've had carriers like Aetna Inc. pull out of the ACA market and we've gone from 11 or 12 [carriers] a few years ago ... down to eight," White said in an interview with S&P Global Market Intelligence.
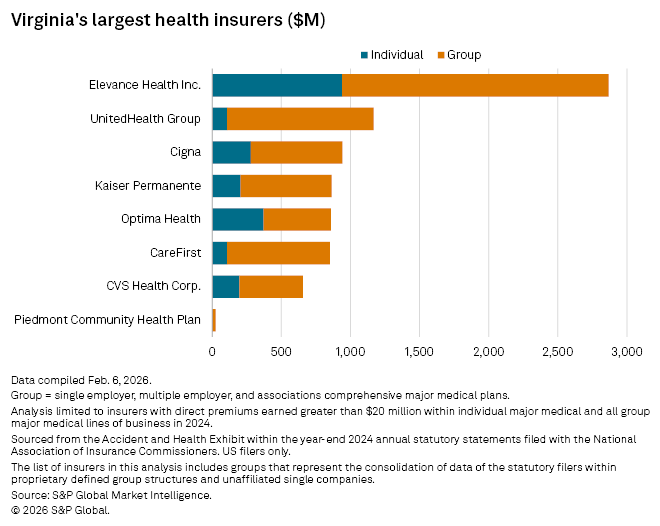
Elevance Health Inc. is the largest health insurer in the state with $2.87 billion in direct premiums earned. UnitedHealth Group Inc. is second with $1.17 billion, followed by The Cigna Group with $941.48 million, Kaiser Permanente Inc. with $862.65 million, Optima Health Corp. with $857.9 million and CareFirst Inc. with $851.1 million.
'No pathway' for Aetna
Aetna's departure from the ACA market, announced by CVS Health Corp. CEO David Joyner during an earnings call, affected 17 states and approximately 1 million subscribers, with almost 400,000 of them from Virginia, according to White.
|
Scott White, Virginia insurance commissioner, NAIC president. |
Other insurers have scaled back Medicare Advantage offerings. UnitedHealth announced on Oct. 1, 2025, that it was exiting Medicare Advantage plans in 109 counties starting in 2026, while Humana Inc. announced later that month that it was exiting two states and 194 counties.
Joyner, during CVS Health's earnings call, said "continued underperformance from our individual exchange products" showed that "there is not a near- or long-term pathway for Aetna to materially improve its position in this product."
"Despite our multiyear efforts, we must recognize what is and what is not working and we'll focus on the areas where we have a clear right to win," Joyner added.
Subsidy expiration effect
The effects of the lost subsidies will be felt in the form of higher premiums for policyholders, White said. Rates have risen 20% due to higher utilization, increased hospital and pharmacy costs, and the anticipated expiration of the subsidies.
"That creates sicker people staying in the pool, healthier ones leaving," White said. "That's what we call that morbidity factor that led to a portion of the increase."
To reduce consumers' premiums, Virginia started its Commonwealth Health Reinsurance Program in 2023. The program, granted through a Section 1332 innovation waiver written into the ACA, has lowered premiums by 15%, while reimbursing carriers for high costs.
With the subsidies expiring, a family of four in Virginia with a household income of $70,000 could see its premiums double, White said, leading to decreased enrollment.
"The trends are that it will be lower in Virginia, just as in any other state, and you can understand why when you see the impacts of the expiration of these enhanced subsidies," White said.
Now, it is a case of waiting to see how the loss of subsidies affects enrollment.
"Once people get their premium renewals ... you could see through February, March and April, the enrollment numbers continue to dip," White said.